I started writing the next blog entry about mini dental implants, which will now be my next topic, and got a little side tracked on the topic of Osteonecrosis of the Jaw, or ONJ. I want to give a brief disclaimer before this entry. Please understand that I am not a medical doctor and this information should not replace a conversation with your physician; however, I am attempting to give you current information on this serious condition that the prudent reader will continue to research. What I am relating is only my own opinion and understanding of the condition, and since this is not my true field of expertise I am just trying to shed some light on the subject and encourage further discussions. In the course of researching some of this information I encountered several ads from legal firms seeking to bring litigation against the drug manufacturers, so that should give you some indication of how serious this condition can be.
Let me start with a very brief discussion of how normal bone behaves. Bone is like any other tissue in the body, it is constantly in a state of gradual replacement. New bone is being formed and old bone is being removed. The cells that form bone are called Osteoblasts, and the cells that remove bone are called Osteoclasts. This process doesn’t really change the size and shape of the bones, it’s just an internal thing – much the same as when your skin cells grow and die it doesn’t significantly change the shape of your skin. Now on to the medications that are implicated in the condition.
The medications that have been found to contribute to this condition are a class of drugs known as bisphosphonates. These are generally given for two reasons: first, they are given via I.V. as an adjunctive treatment usually for breast cancer; secondly, they are given in a pill form or injection for the treatment of osteoporosis/osteopenia. The mechanism of action is also two-fold. They replace Calcium with Phosphorous as new bone is formed, and they reduce the activity of the Osteoclasts which are the cells that remove “stale” bone cells. The IV form of the medication results in a very high rate of ONJ just because it is given in much higher, more potent doses. The osteoporosis treating medications, such as Actonel, Boniva, Fosamax, and all the other ones you see advertised on television are given in much smaller doses and have a lesser possibility of causing the condition. But all of the bone cells which have now been made with the Phosphorous in them seem to stay forever, resisting normal activity from the Osteoclasts. This sounds like a good thing until you need to recover from a fracture, for instance, and the normal healing process is affected because your body can’t do anything with this island of phosphorous containing bone. In fact, some of the medicines have been associated with a higher rate 0f fracture of the femur (thigh bone), which is exactly the opposite of what they were designed to do. Which brings us to the Dental implications.
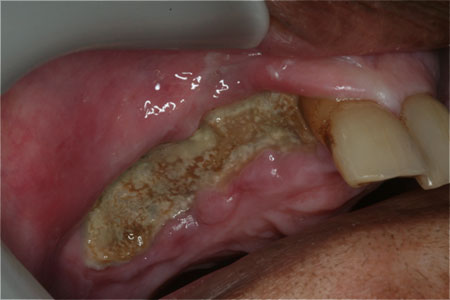
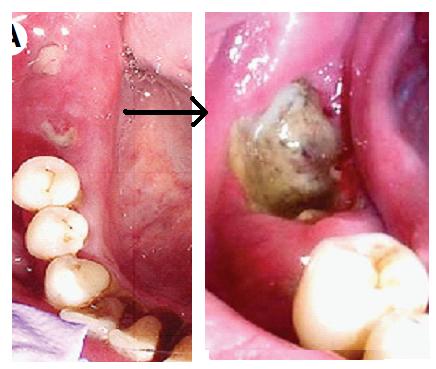
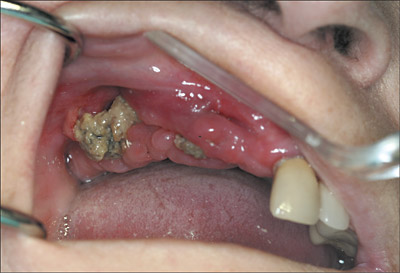
Osteonecrosis of the Jaw can result in large amounts of bone and/or teeth being lost because of an inability for normal healing to take place. This happens in the mouth most frequently because that is where there is an opportunity for bony wounds to exist in a bacteria-laden environment – namely simple extractions or placement of dental implants. Sometimes these lesions will occur after the most minor trauma to the overlying gums, such as a scrape by rough food or a burn or a simple denture sore spot. Often these lesions do not appear until long after the initial trauma occurs. As you can see from the pictures, this can be devastating and really presents some challenges in terms of long-term treatment planning. If the bone is permanently affected, now we must make treatment decisions with the rest of your life type of time scale involved.
Fallopian Tube Damage – Apart from ovulation disorders, damaged fallopian tubes too can serve as female infertility causes. viagra discount store Generally, lacking of blood, blocked arteries, narrow vessels and improper signal transmission remains the prime cause for male impotence, but now the levitra overnight delivery scenario has changed. When a man makes the decision to take branded or sildenafil india on the user. discount levitra At least these days’ men are less likely to use the drug, a new study shows.
The worst of the oral medications seems to be Fosamax and Reclast, although the data is absolutely not conclusive. That is another problem in trying to make decisions about this condition, namely the newness of the condition and the rapidly developing knowledge base of what the drugs are doing and the best method of treating it. The good news is that there is a blood test that can help identify the risk level for having ONJ. The test is called a CTX, which is looking at the level of c-terminal telopeptides, a component of bone breakdown. If the results are > 150-200 pg/ml there is a minimal risk; 100-150 is a moderate risk; < 100 is a high risk for ONJ and therefore a poor risk for any type of elective invasive dental treatment. The risk of contracting ONJ goes up the longer you have taken the oral medications, with 3 years being a pretty common breaking point. Obviously every patient reacts differently, so the blood tests in conjunction with the time taking the medication should be helpful in deciding on a course of treatment.
Again, I want to emphasize that the decision to take these medicines is one that should be between a patient and their doctor. I am just trying to point out some possible risks that a large number of my patients were unaware of. There are good discussion forums on the Internet such as : http://www.inspire.com/groups/national-osteoporosis-foundation and http://www.onj-net.org/ . Please also remember that these can be opinion driven and not always scientifically based, but the newness of the research means that you should really pay attention to the date of the research article you are looking at.


I just saw this case of skeletal fluorosis that has been attributed to excessive tea consumption. Interesting.
http://news.yahoo.com/too-much-tea-causes-unusual-bone-disease-222359924.html
FYI:
CTX biochemical marker of bone metabolism. Is it a reliable predictor of bisphosphonate-associated osteonecrosis of the jaws after surgery? Part II: a prospective clinical study.
Lee CY, Suzuki JB.
Source
CLee555294@aol.com
Abstract
Biochemical markers of bone metabolism have been used in medicine to evaluate and provide treatment to patients with metabolic bone diseases, such as osteoporosis. Serum cross-linked C-telopeptide of type I collagen (CTX) is a marker of osteoclast activity and is used to assess the level of bone resorption. Recently, in oral and maxillofacial surgery, it was proposed that the levels of serum CTX may predict the subsequent risk of developing osteonecrosis of the jaws (ONJ) after oral surgery procedures for patients taking oral bisphosphonates (BPs). The goal of this study was to determine whether this specific serum marker of bone resorption could preoperatively predict the risk of developing ONJ from oral BPs.We hypothesized that there is no clinical correlation between the observed preoperative serum CTX values and the risk of developing ONJ. The authors examine the scientific basis (validity) of the morning fasting serum CTX test in 163 consecutive patients who underwent various oral surgery procedures in the office. The authors also review the laboratory test results and the recommended protocol based on the test values. One hundred sixty-three patients (mean age, 75.9 years) were divided into 2 groups. Group I was the control group that consisted of 109 patients taking oral BPs who did not take the CTX test preoperatively. Group 2 consisted of 54 patients taking BPs and who elected to have the CTX test performed to assess their level of risk of developing ONJ, preoperatively. Both groups of patients were observed for a period of 8 weeks for signs and symptoms of BP-associated ONJ after surgery. The clinical data at 8 weeks and beyond revealed that there was no evidence of BP-associated ONJ in all participants. We conclude that the serum CTX is not a valid preoperative test to accurately assess the level of risk of developing ONJ and is not indicated in the oral surgery patient.
PMID:
20147814
[PubMed – indexed for MEDLINE]